Researchers are still learning why some people recover quickly from COVID-19 while others experience lasting symptoms for months or years. This lingering illness — known as Long COVID or post-COVID syndrome — can affect many body systems and disrupt daily life. A new study from The University of Texas Health Science Center at San Antonio offers important clues about who is most at risk and why.
What is Long COVID?
The National Institutes of Health defines Long COVID as symptoms that last or appear at least four weeks after a COVID-19 infection. These can include:
- fatigue
- shortness of breath
- brain fog
- chest pain, and
- loss of smell or taste
For some, the symptoms fade over time. For others, they persist and interfere with work, relationships, and health.
A study of over 23,000 people
The study, published in JAMA Network Open in January 2025, analyzed data from more than 23,000 participants in the NIH RECOVER Initiative (see sidebar).
Researchers led by Dr. Dimpy P. Shah of the University of Texas Health Science Center, San Antonio, looked for patterns that might explain differences in the risk of Long COVID between men and women. They studied both people who had COVID-19 and those who didn’t, using medical records, lab tests, and detailed symptom surveys.
About the RECOVER Initiative
The NIH Researching COVID to Enhance Recovery (RECOVER) Initiative is a nationwide research program launched in 2021 to understand the long-term effects of COVID-19. It brings together scientists, clinicians, and patients from across the United States to identify who is at greatest risk of Long COVID, why symptoms persist, and how to treat or prevent them. By collecting data from tens of thousands of participants, RECOVER aims to speed the discovery of therapies that can help people return to full health after COVID-19.
Key findings: Women are more likely to develop Long COVID
The researchers found that women have a higher risk of Long COVID than men. Women reported more persistent symptoms and more interference with their daily activities.
The association between sex and the risk of Long COVID was not uniform. It depended on age, pregnancy, and menopausal status. In fact, the higher risk for women did not show up significantly in the 18-to-39 age group. That suggests that in younger adults, men and women had more similar long COVID rates.
When the researchers excluded people who were pregnant, the risk of Long COVID in women was even stronger. Among participants aged 40 to 54 years, women who were not yet menopausal had a 1.45-fold higher risk compared to men. Even menopausal women in that age bracket had elevated risk (though more modest) in comparison to men.
These results suggest the risk of Long COVID among women is highest in midlife, particularly between 40–54 years. They also highlight that hormonal and biological factors may strongly shape long-term outcomes after COVID-19 infection.
Men, in contrast, were less likely to develop Long COVID but more likely to experience severe symptoms during the initial infection. The researchers believe these patterns could reflect biological and hormonal differences. These differences may shape how men and women respond to the virus and how their symptoms evolve over time.
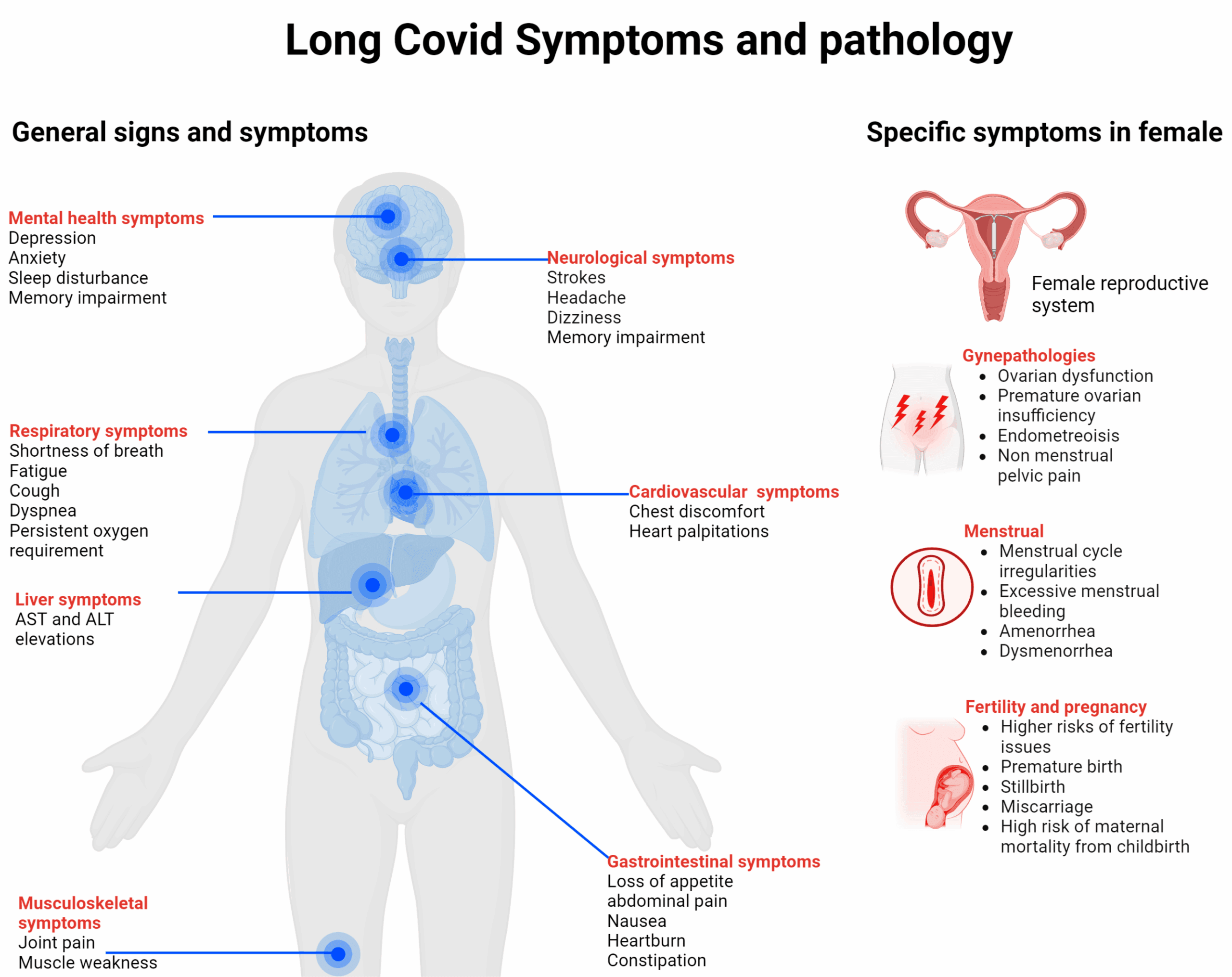
From Maham S, Yoon M-S. Clinical Spectrum of Long COVID: Effects on Female Reproductive Health. Viruses. 2024; 16(7):1142. https://doi.org/10.3390/v16071142 shared under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Understanding why these differences matter
Dr. Shah and her team emphasized that the risk of Long COVID varies widely across individuals. By identifying which factors contribute to that risk, scientists can target prevention and treatment efforts.
The findings also suggest that sex-based differences should be considered in how Long COVID is diagnosed and managed. For example, symptoms like fatigue and brain fog may be overlooked or misattributed, especially in women. Understanding these nuances could lead to more personalized care.
The new study underscores that the risk of Long COVID is not the same for everyone. Women appear more vulnerable, and understanding why could be key to finding effective treatments. As research continues, these insights bring us closer to helping all people recover fully from COVID-19.
What’s next for research
Future studies in the NIH RECOVER program will look more deeply at biological mechanisms — such as hormones, genetics, and immune system activity — that might explain the sex differences in the risk of Long COVID. Researchers will also explore how these differences evolve over time and how treatment responses vary by sex.
The ultimate goal is to identify ways to prevent Long COVID altogether — or at least lessen its long-term effects. This will require collaboration among scientists, clinicians, and patients across the country.
The Parsemus Foundation supported enrollment efforts for several clinical trials of drugs for COVID-19 treatment, including the COVID-OUT study. The study found that metformin, a common diabetes drug, reduced serious outcomes for COVID-19 infection, including the incidence of Long COVID. See our COVID-19 project page here. See our other news articles about COVID-19 here.